Provincial officials found five violations of the Fixing Long-Term Care Act during an inspection carried out at Leacock Care Centre in June.
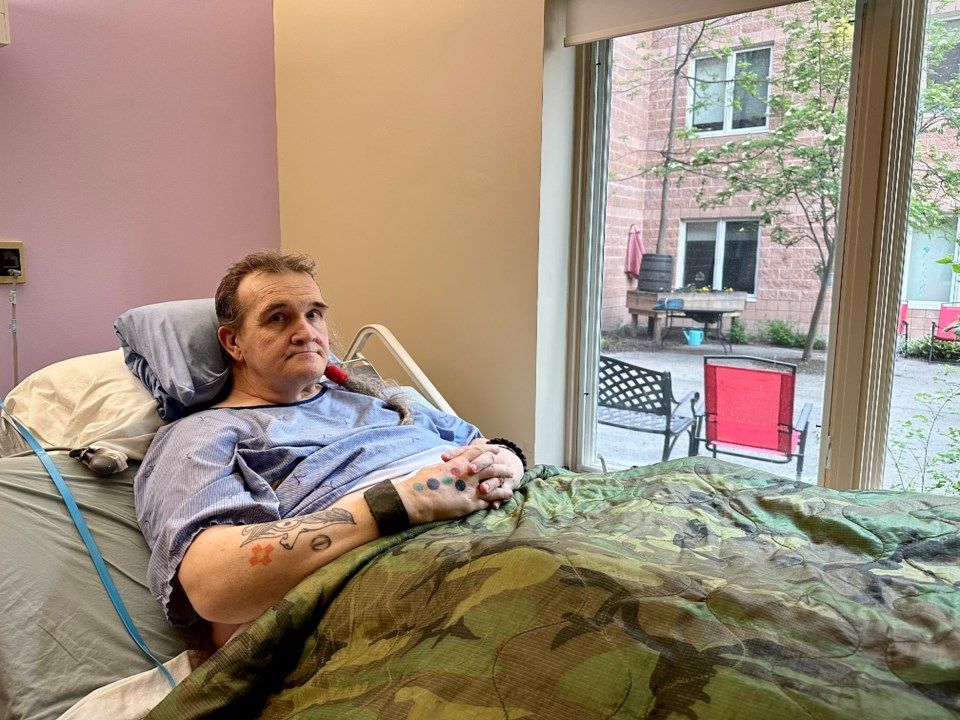
The inspection followed OrilliaMatters’ coverage of an incident involving resident Dav Langstroth, who had been left in his waste overnight due to staffing issues at the Orillia long-term care home in May.
The inspection, carried out by the Ministry of Long-Term Care, took place across seven on- and off-site visits between June 7 and 19, finding five instances of non-compliance with the act in relation to three residents at the home.
For one resident, identified as resident #003 in the report, the ministry found the home failed to protect the resident from neglect as “care was not provided to the resident for an extended period of time,” resulting in “moderate impact and risk to the resident.”
The ministry also found the home failed to identify the level of assistance required in the resident’s plan of care, with regard to the resident’s continence care, and that it failed to implement a “specified intervention” in several instances of the resident’s care.
For residents identified as #001 and #002, the ministry found the home failed to provide the appropriate amount of continence care to ensure they were “clean, dry and comfortable,” and that specified products for continence care were not provided to them.
The home also failed to ensure resident #001’s specific continence care requirements were included in the plan of care.
As per the report, the ministry stated the plans of care for residents #001 and #002 were updated prior to the conclusion of the inspection.
During the inspection, Langstroth said, he was visited by the ministry inspector and recounted the May incident, when he was left in his waste between the hours of 10:30 p.m. May 22 and 6 a.m. May 23.
“I told her what happened. I pushed on her the fact that the staff were very concerned about my care, but had no one available to come and help me. That’s just the bottom line,” he said, “and that (for) the morning staff, I was their priority. However, their priority didn’t happen until 6:30 in the morning (and) they come on at six.”
Langstroth found the level of care he received improved greatly over the month following the incident, but he said that level of care has not been upheld over the summer.
“For about a month afterwards, I would get somebody at my door, when I hit the call bell, usually within 30 seconds,” he said. “Since that month has passed, it’s getting more and more ... 15 minutes, half an hour, 45 minutes.”
While he has said workers generally do their best to provide him with care, he expressed concerns with staffing issues throughout the province’s long-term care system.
The Fixing Long-Term Care Act prescribed a goal of providing long-term care residents with three hours, 15 minutes of care per day by March 31 — a threshold Langstroth does not believe is being met.
“In this building, each resident is required to have 3.25 hours of care per 24 hours. Do the math. How many people do you need in order to do that? There aren’t enough,” he said. “They are unable to do that. The reason is they can’t get enough people to do the job.”
Langstroth said he has committed to being a voice for residents who cannot speak out for themselves.
“I have no ability to make change. However, what I can do is ensure that the people who can’t speak have a speaker on their behalf,” he said. “Those that don’t know who they are, where they are, what they’re doing, why they’re here — a lot of them are crying because they figure that they’ve been abandoned.”
Trevor Sykes, community relations co-ordinator for Jarlette Health Services, which runs the Leacock Care Centre, said providing quality care to its residents is the top priority.
“The primary concern of Leacock Care Centre, each and every day, is the health, safety and well-being of our residents,” Sykes told OrilliaMatters. “We are committed to implementing any measures prescribed by the Ministry of Long-Term Care.
“We remain in close direct contact with the resident, and indeed every resident, to ensure their needs are properly met.”
Sykes said Jarlette works closely with health-care and provincial partners to ensure residents “receive the best possible care, often implementing policies and programs beyond those required by our ministry partners.”
He noted the province is currently experiencing a “health human resource crisis,” but ensured Leacock is fully staffed.
“We are able, however, to remain fully staffed, including if necessary through the use of recruitment agencies,” he said. “For further information about the health human resource crisis which is impacting long-term care homes and the broader health-care sector across Ontario, I recommend reaching out to the Ontario Long-Term Care Association directly or the Ministry of Long-Term Care.”
The ministry’s report on the Leacock Care Centre can be found here.